Do you know your risk for hereditary breast cancer?
“There are many high-risk women out there who may not even realize they’re high risk,” says Terri Imada, nurse practitioner at Queen’s Cancer Center.
Imada opened the first high-risk breast cancer program in Hawaii 16 years ago. She and genetic counselor Sam Bailey care for patients dealing with hereditary cancer indicators like BRCA mutations, which cause high breast and ovarian cancer risk.
Imada and Bailey share their expertise in hereditary cancer, what a BRCA mutation means, and what to do if you think you’re at risk.
How do you know if you’re at high risk for hereditary cancer?
SB: Start with encouraging discussion in your family. Think about things you hear ― that uncle or auntie so-and-so had cancer. It’s important to ask detailed questions like:
- What type of cancer did they have?
- How many people in your family have had cancer?
- Is it the same type of cancer?
- Did someone have cancer at a young age?
These are the things you should talk to your doctor about. Not all primary care providers are asking detailed questions about this. If they don’t get that information from you, you may not be recognized as high risk.
How do BRCA gene mutations elevate breast and ovarian cancer risk?
SB: Genes are sets of instructions for your body to do certain things. In the case of the BRCA1 and BRCA2 genes, they’re tumor suppressors. A mutation, or difference, in the BRCA gene means that you have a copy that’s not working, which can result in higher cancer risk.
We all acquire DNA damage throughout our lifetime that can elevate our cancer risk. But with hereditary cancer, you're starting off with an inherited change in the DNA that puts you closer to the point where that cell could become cancerous.
How can you find out if you have a BRCA gene mutation?
SB: Talk to your PCP about meeting with a genetic counselor. You and your counselor will discuss whether genetic testing is appropriate for you. After pretest counseling, you’ll take a blood test. It takes about three weeks to get results.
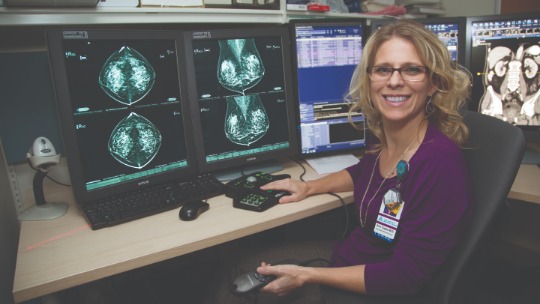
Erin Capps, MD, board certified radiologist, reviews breast radiology images
What does it mean if you test positive?
TI: If you have a BRCA mutation, your breast cancer risk can be 4 to 7 times higher than the average women. Your risk for ovarian cancer can also be significantly elevated.
For breast cancer, you have options. The first is you can start screening closely. High-risk breast cancer screening starts at age 25. For the first five years, that’s yearly MRIs. From 30-75, it's MRIs and mammograms.
The second is you can choose to surgically remove the breasts with or without reconstruction. We know that this surgery gives you a 90-95% risk reduction for breast cancer.
The same is true for ovarian cancer. You can opt to remove the ovaries, fallopian tubes, and uterus as a preventive measure or you can start high-risk screening with transvaginal ultrasounds and blood tests. Sensitive counseling is essential because these are tough choices for women to make.
What does it mean if you test negative?
SB: There’s a misconception that if you test negative, you’re fine. If you have a family history of breast cancer, that’s notable no matter what. Even if the BRCA mutation has been addressed through genetic testing, you’re still at high risk and you may want to do more screening.
TI: A lot of high-risk women who have family histories need different care and monitoring. You may still qualify for yearly mammography, yearly breast MRIs, and preventive drugs to lower your cancer risk.
If you think you’re at risk or need help navigating hereditary cancer, visit the Queen’s Cancer Center website or call (808) 691-8777.
Hero photo: Hal Lum and Masayo Suzuki
Photo of Dr. Capps: Queen's Cancer Center




